As an Indigenous midwife at K'Tigaaning Midwives in Nipissing First Nation in Canada’s North Bay, Ontario region, Emily Chartrand-Hudson takes a trauma-informed approach while delivering care. Helping women and families in her community heal from historical and ongoing trauma, addictions and racism and putting them on a path to good health and well-being is core to what she does every day.
“Intergenerational trauma is real,” says Chartrand-Hudson. “Looking at things from a trauma-informed lens makes you more sensitive to the socio-economic, cultural and lifestyle factors that stem from it. It is very meaningful for people to feel understood by the people taking care of them. With that cultural awareness and sensitivity, we can really meet people where they are, and provide them with care that feels better for them.”
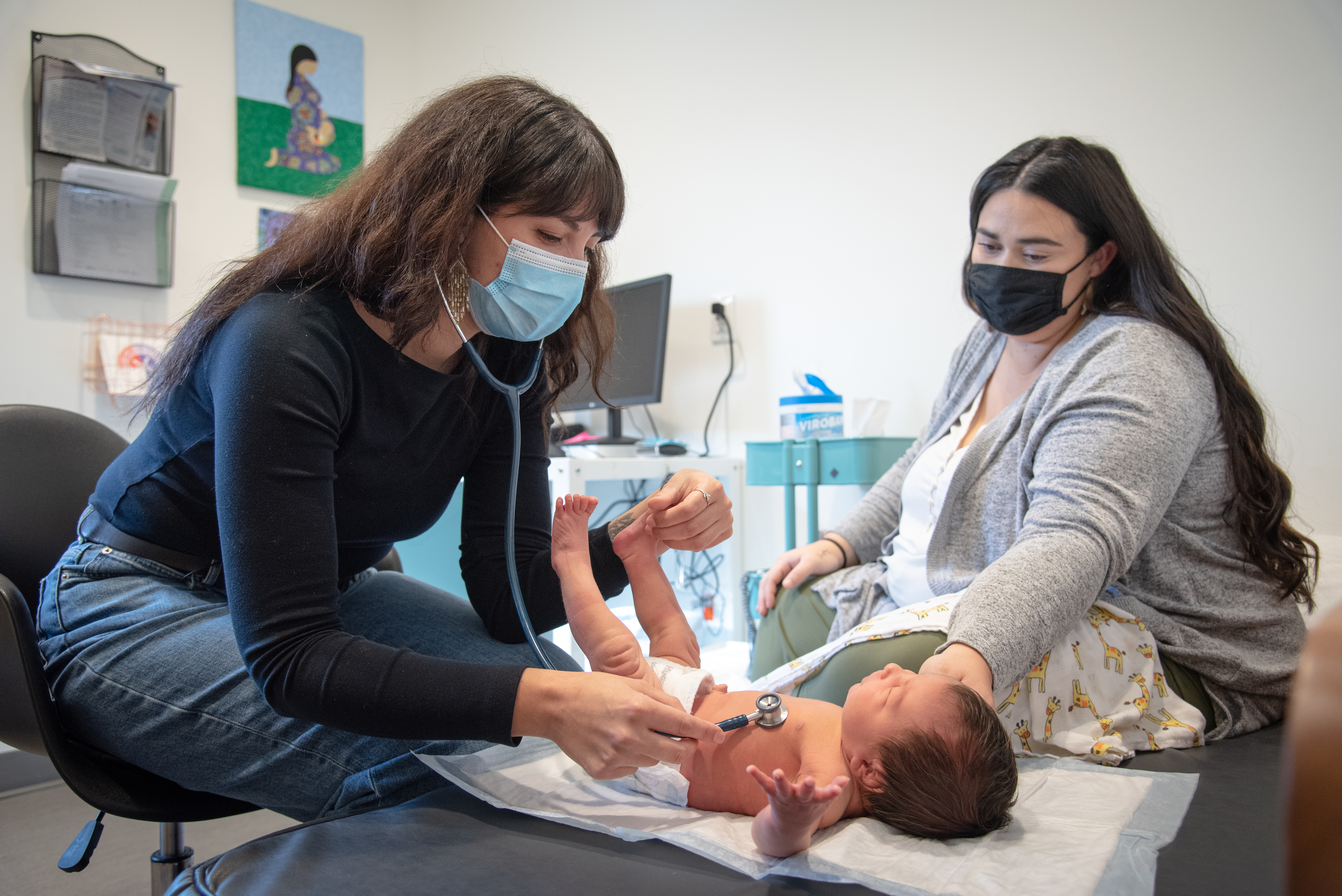

Most of the year Chartrand-Hudson is based in North Bay, providing both care in client's homes and care in the clinic that is located on the reserve just outside the city. Midwives are expected to be proficient in both hospital deliveries and out of hospital home or clinic deliveries, she says. “We go wherever people need us.”
And the need is even greater in remote communities where the majority of Canada’s Indigenous population lives. In many such communities, birth evacuations between 36 and 38 weeks of pregnancy—strongly condemned as racist and continuing the trauma of colonization—is still routine practice.
For two months out of the year Chartrand-Hudson flies out to work on the Attawapiskat First Nation reserve in the far north that is not accessible by land during the winter. Healthcare is limited to a nursing station staffed by a handful of nurses and nurse practitioners, a rotation of midwives like Chartrand-Hudson who spend 1-3 months at a time there, and doctors who fly up on occasion.
“Health outcomes are poor because there aren’t a lot of health providers or access to emergency services,” notes Chartrand-Hudson. In Canada, Indigenous populations are at substantially higher risks of adverse birth outcomes, with mortality rates for Indigenous infants two to four times higher than the national average.
“I became a midwife because of my mom.”
Her mother was 16 when Chartrand-Hudson was born—not uncommon in Indigenous communities. “She had a conventional hospital birth and experienced a bunch of complications, some of which were not within her control and some of which I feel were in part due to racism, and the way the hospital system would have treated a teenage mom,” notes Chartrand-Hudson.
That experience and the next hospital birth led her mother to have a home birth with a midwife for her third child. Chartrand-Hudson was eight at the time and recalls being very interested and wanting to be a part of everything that was happening. While the rule of thumb is for two registered midwives to be present at every home birth, the rural community where they lived at the time only had one midwife. The midwife was accompanied by a second attendant, usually a lay person, sometimes with some nursing experience, who acted as a second pair of hands in the event of an emergency.
“Our neighbor happened to be the second attendant, and when she saw how excited I was she made me her little helper,” Chartrand-Hudson recalls. “I was tasked with being the ‘cold cloth fetcher’ to cool my mom’s forehead. When the baby's head crowned, she was like, ‘come in here and watch this, I'm going to explain to you what's happening.’ I just loved it and was bouncing around the house so excited when my sister was born. I just thought it was so cool.”
Treating childbirth as a sacred event
She draws on her mom’s story and the strengths of the Indigenous culture to empower the people in her care. “Taking care of teenage clients is my very favorite thing to do, I have a soft spot for them that comes from my love for my mom. People judged her and thought she wouldn’t be able to go to school when she became pregnant at 16. But she graduated high school, went to college, had more kids, still kept going to college. She worked as a social worker and made a very good life for us.”
Indigenous pregnant people tend to have more complex pregnancies, Chartrand-Hudson notes. “Higher rates of gestational diabetes, obesity, hypertension can be a bit more common, but I think the major issue is that they tend not to be treated respectfully.”
Chartrand-Hudson remembers a 16-year-old client who flew down from one of the coastal communities and came to their practice because she did not want a hospital birth. If she stayed in her community, she would have been evacuated during the last month to give birth.
The young client brought her whole family with her, including her grandmother who made traditional meals, and her father, brothers and boyfriend who kept a fire going and were drumming and singing while she went into labor, providing a sacred circle of support through the whole process. “It makes me teary thinking about it. She had the most beautiful water birth supported by the people who loved her. She was so euphoric and so determined to succeed.”
This is the kind of difference Indigenous midwives can make, and why Chartrand-Hudson is passionate about ensuring access to midwifery care in Indigenous communities. Even in North Bay where she works for much of the year, there are only four or five midwives in that urban community. “We have huge waiting lists all the time and turn away a lot of people because we cannot accommodate them.”
Creating pathways for Indigenous midwifery education


The National Aboriginal Council of Midwives (NACM) is committed to bringing back the knowledge, skills and leadership of Indigenous midwives, once a cornerstone of every Indigenous community, but lost as a result of colonization and ongoing systemic racism in the Canadian healthcare system.
In 2019, funded by Johnson & Johnson Canada, NACM developed the competencies framework, Indigenous Midwifery Knowledge and Skills, to better understand and meaningfully grow Indigenous midwifery. Building on this work, the Johnson & Johnson Center for Health Worker Innovation, with support from Johnson & Johnson Foundation, began collaborating with NACM in 2021 to advance an Indigenous-led initiative to diversify pathways to midwifery education as part of a broader strategy aimed at growing and sustaining Indigenous midwifery in Canada.
The design innovations being developed, implemented and evaluated include expanding community-driven, competency-based Indigenous midwifery education through an apprenticeship model that brings Indigenous midwifery education as close to home as possible as well as new learning options for Indigenous midwifery students in university-based midwifery education programs. Overall, the project is grounded in a vision to revitalize, restore and grow the practice of Indigenous midwifery in Indigenous communities in rural, urban and remote areas of Canada. This effort is enabling First Nation communities like Sturgeon Lake First Nation, Saskatchewan, reclaim childbirth in their communities for the first time in 50 years.
While in midwifery school, Chartrand-Hudson was the student representative for NACM and became a core leader for one year after graduation. With Canada’s Indigenous population growing four times faster than the rest of the country, Chartrand-Hudson is a strong advocate for paving pathways for Indigenous midwifery education. As a NACM member, she is working to ensure that every Indigenous community has Indigenous midwives and every Indigenous woman can safely give birth close to home and rooted in their culture.

